Why do some behavioural patterns seem “out of place,” unusually intense, or difficult to understand?
Why do some people struggle to maintain relationships, regulate their emotions, or cope with everyday stress, even when they’re genuinely trying?
In some cases, these struggles may be linked to personality disorders, which are long-term and deeply rooted patterns of thinking, feeling, and behaving that can shape how a person views themselves, interprets the world, and responds to the people around them.
Personality disorders are not simply occasional mood changes or short-term reactions to stress. They are enduring traits that begin in adolescence or early adulthood and remain consistent across different situations. By understanding what these disorders are, how they’re categorised into Cluster A, B, and C, and the symptoms and treatment options available, we can better appreciate the challenges individuals may experience. This insight not only improves awareness but also encourages compassion, early support, and informed decision-making.

What Are Personality Disorders?
Personality disorders are long-term mental health conditions that involve rigid and unhealthy patterns of thinking, feeling, and behaving. These patterns significantly deviate from cultural norms and make it challenging for an individual to interact with others or manage their daily life.
Distorted beliefs, strong or erratic emotions, and trouble controlling their reactions are common in people with personality disorders. This may have an impact on how they view themselves, how they understand circumstances, and how they act in interpersonal or stressful situations.
Types of Personality Disorders
Personality Disorders are mainly divided into three main types: Cluster A, Cluster B, and Cluster C. Each cluster is unique in its own way of thinking and interpreting the world. Understanding these three types of clusters helps us to identify how these disorders present differently and how they affect day-to-day lives.
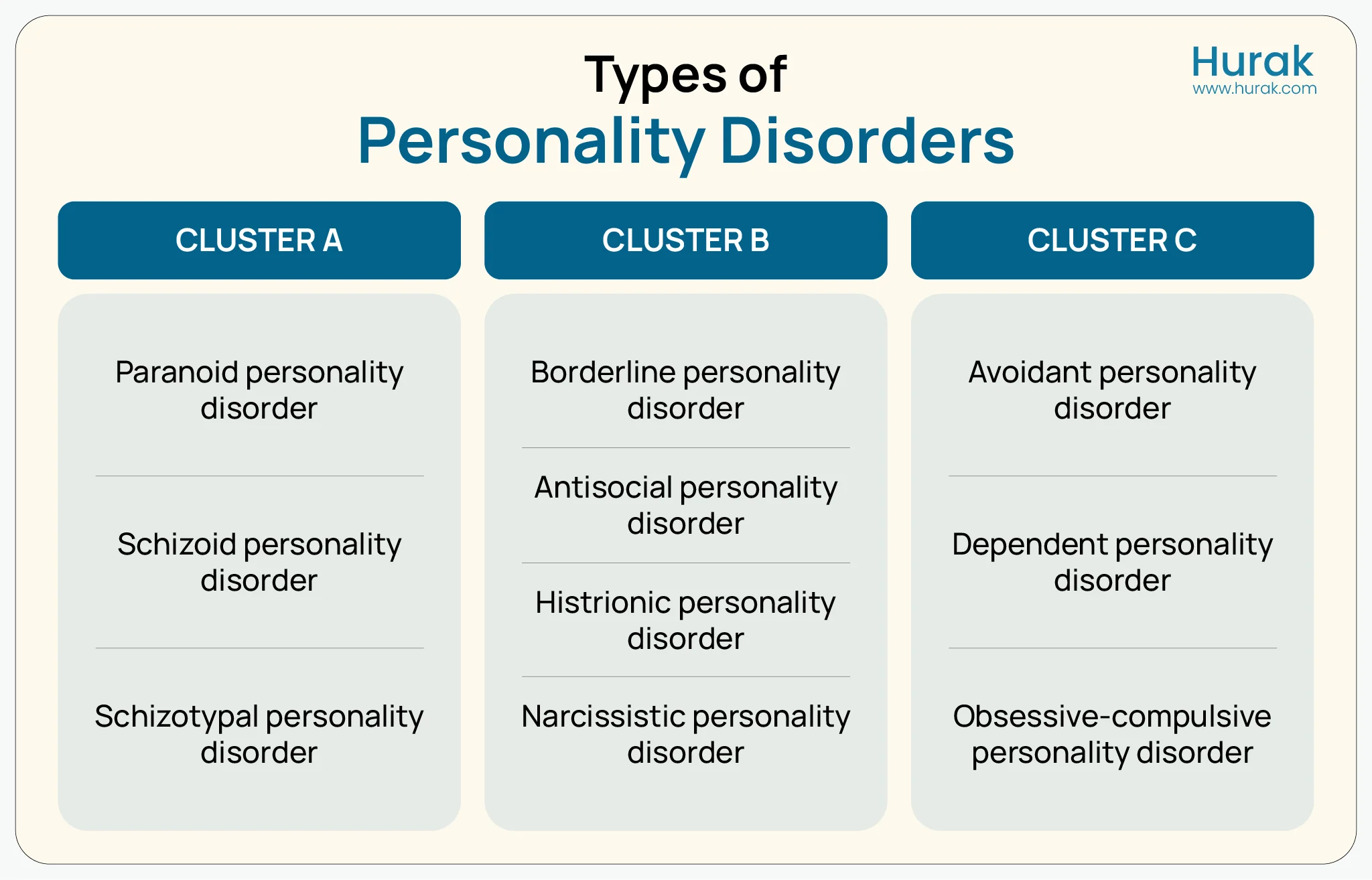
1. Cluster A Personality Disorders
Cluster A personality disorders involve unusual thinking patterns, social withdrawal, and difficulties forming close relationships. People may appear eccentric, suspicious, or emotionally distant.
Cluster A includes:
Paranoid Personality Disorder (PPD)
People with PPD exhibit a recurring pattern of mistrust and suspicion. They often tend to think that others lie, manipulate, or are out to harm them, even without evidence. This complicates their ability to relate closely with others since they can perceive the least harmful things as threats or insults. It is also characterised by emotional detachment, hostility, and a state of vigilance.
Schizoid Personality Disorder (SPD)
Individuals with SPD typically prefer being alone and show limited emotional expression. They often look impersonal, cold or even don’t care about social interactions. They rarely seek closeness or approval and may find it difficult to experience happy moments. Being alone does not make them upset; this is just their style of life.
Schizotypal Personality Disorder (STPD)
People with STPD are characterised by strange beliefs, peculiar perceptions of reality, and odd behaviours. Magical thinking, belief in special powers, or interpretations of events may occur in people in a particular way. They often feel uncomfortable in close relationships and may struggle with social anxiety. Their speech or appearance may seem unusual, and they may misinterpret social cues.
2. Cluster B Personality Disorders
Cluster B includes disorders characterised by intense emotions, unstable relationships, impulsivity, and dramatic behaviour.
Cluster B includes:
Borderline Personality Disorder (BPD)
BPD involves unstable emotions, self-image, and relationships. Individuals may have intense mood swings, fear of abandonment, and impulsive behaviours such as self-harm or risky decisions. Their relationships can shift rapidly from closeness to conflict, leaving them feeling empty, misunderstood, or overwhelmed.
BPD is also known as emotionally unstable personality disorder (EUPD) and emotional intensity disorder (EID).
Antisocial Personality Disorder (ASPD)
People with ASPD frequently violate other people’s rights, break the law, and exhibit a lack of regret. They could be dishonest, cunning, violent, or careless. Although criminal behaviour is frequently associated with this disorder, not all people with ASPD commit crimes. Two fundamental characteristics are persistent rule-breaking and difficulty empathising.
Histrionic Personality Disorder (HPD)
Individuals with HPD display excessive emotionality, dramatic expression, and a constant need for attention. They may use their appearance, speech, or behaviour to draw attention and may feel uncomfortable when not in the spotlight. Their emotions can be shallow but intense, and relationships may feel superficial or overly dependent on approval.
Narcissistic Personality Disorder (NPD)
NPD is characterised by grandiosity, a strong need for admiration, and limited empathy. People may believe they are superior, expect special treatment, and struggle to recognise the feelings or needs of others. Despite appearing confident, they often have fragile self-esteem and may react strongly to criticism.
3. Cluster C Personality Disorders
Cluster C disorders involve persistent fear, worry, and avoidance. People often appear overly anxious, self-conscious, or dependent on others.
Cluster C includes:
Avoidant Personality Disorder (AvPD)
Individuals with AvPD experience intense sensitivity to criticism and rejection. They want social connections but avoid relationships out of fear of embarrassment or failure. Low self-esteem, social withdrawal, and constant worry about being judged are common features. This fear often interferes with work, friendships, and daily life.
Dependent Personality Disorder (DPD)
DPD involves an excessive need to be cared for, supported, or guided by others. People may rely heavily on partners, family, or friends for reassurance and decision-making. They fear being alone, struggle with confidence, and may tolerate unhealthy relationships to avoid separation.
Obsessive-Compulsive Personality Disorder (OCPD)
OCPD is defined by rigid perfectionism, orderliness, and control. Individuals may set extremely high standards for themselves and others, leading to stress, frustration, and difficulty delegating tasks. Unlike OCD (Obsessive-Compulsive Disorder), which involves intrusive thoughts and compulsions, OCPD focuses on personality traits such as inflexibility, excessive organisation, and strict routines.
By understanding the three clusters and their unique traits, we can identify early signs and encourage timely help. Personality disorders may be long-term, but effective treatment and support can greatly improve quality of life.
Looking to deepen your understanding of personality disorders?
Our Mental Health First Aid (MHFA) course provides essential knowledge and practical skills to promote well-being in everyday situations. Build the confidence to help someone when they need it most.
Symptoms of Personality Disorders
Personality disorder symptoms can vary widely, but they usually involve long-term patterns of thinking, feeling, and behaving that make everyday life harder. These symptoms often show up in relationships, emotions, self-image, and decision-making.
Common symptoms include:
1. Difficulties in Thinking and Perception
- Seeing situations in rigid or extreme ways
- Misunderstanding the intentions of others
- Having unusual beliefs or strange ideas
- Having trouble interpreting social cues
2. Emotional Challenges
- Strong or quickly shifting emotions
- Inability to control emotions under pressure
- Feeling empty, insecure, or easily overburdened
- Overreacting to small disagreements or criticism
3. Behavioural Difficulties
- Impulsive or dangerous actions
- Avoiding social situations out of mistrust or fear
- Controlling, dramatic, or attention-grabbing behaviours
- Having trouble upholding responsibility or adhering to rules
4. Relationship Problems
- Having trouble establishing or sustaining positive relationships
- Fear of being rejected or abandoned
- Relationships that are unstable or full of conflict
- Preferring isolation or finding closeness uncomfortable
5. Issues with Self-Image
- An unstable or unclear sense of identity
- Excessive self-importance or low self-esteem
- Continuous need for approval or reassurance
- Feeling cut off from oneself
These patterns might help identify when an individual may be experiencing a personality disorder rather than a temporary complication. The experiences may profoundly influence the way an individual views themselves and others, and how they cope with daily life. Through early identification, sensitive care, and proper management, people will be able to acquire more rewarding coping strategies and develop more satisfying relationships.
Causes of Personality Disorders
Personality disorders don’t have a single cause. In most cases, they build slowly, over the years. Different things mix together, such as family background, early experiences, the environment someone grows up in and all of it quietly shapes how a person sees themselves and the world.
Genetic Factors
Genetics can be part of this, though it’s not as simple as “it runs in the family.” Some people are born more emotionally sensitive, more reactive, or more anxious by nature. That doesn’t mean anything is wrong with them. And it doesn’t mean a disorder is guaranteed. But when those traits meet stress, instability, or emotional neglect, things can start to feel harder to manage.
Childhood Trauma & Adverse Experiences
Childhood experiences matter a lot here. Especially the difficult ones. Growing up with abuse, neglect, constant conflict, or sudden loss can change how a child learns to feel safe. It can affect trust. It can affect emotions. And when those early experiences aren’t processed or supported, they don’t just disappear with age. They often follow a person into adulthood, showing up as fear, emotional intensity, mistrust, or ongoing struggles in relationships.
Brain Structure & Neurobiology
The brain can be part of this, too. Some research shows that the parts of the brain linked to emotions, control, and decision-making don’t always work the same way in everyone. It’s not something you can easily see, but it can affect reactions and behaviour. Brain chemicals matter as well. If things like serotonin or dopamine are off, emotions can feel intense or harder to handle.
Personality & Temperament Factors
Personality matters here. Some people are just more sensitive, reactive, or impulsive from a young age. That’s just how they are. It’s not a disorder by itself. But when stress, trauma, or difficult experiences come into the picture, these traits can make things harder over time.
So there isn’t one clear cause. It’s usually a mix of how someone is wired and what they’ve gone through. Understanding this helps us be less judgmental and more supportive.
Treatment for Personality Disorders: Approaches That Work
When it comes to treating personality disorders, therapy is usually the main thing people start with. It helps them understand their emotions and why they react in certain ways. Over time, it can also help change behaviour patterns that have been there for years. Medicines may be given in some cases, but mostly to help with specific symptoms. Therapy is still the most important part for most people.
Psychotherapy (talk therapy)
Talk therapy is basically about talking things out. It helps people understand their thoughts, deal with emotions better, and improve relationships. There are different types of therapy, and each one works in a slightly different way.
Cognitive Behavioural Therapy (CBT)
BT focuses on thoughts and behaviour. It helps people notice negative thinking patterns and try healthier ways of responding. It’s more practical and focuses on everyday problems.
Dialectical Behaviour Therapy (DBT)
DBT is helpful for people who feel emotions very strongly. It teaches skills to stay calm, handle stress, and control impulsive behaviour. It also helps with relationships.
Mentalisation-Based Therapy (MBT)
MBT helps people understand their own thoughts and feelings, and also those of others. This can reduce misunderstandings and emotional reactions, especially in relationships.
Psychodynamic therapy
This type of therapy looks at past experiences, especially from childhood. It helps people understand where certain patterns come from and why they keep repeating.
Medications
Medication doesn’t really cure personality disorders. It’s mostly used to deal with certain symptoms that can be hard to handle day to day. Things like feeling very anxious, low, impulsive, or having sudden mood changes. For most people, medicine is just one part of treatment, not the main solution.
Antidepressants
Doctors sometimes give antidepressants when someone feels depressed, anxious, or emotionally all over the place. It doesn’t change a person’s personality, but it can help calm things down a bit.
Mood Stabilisers
Mood stabilisers are used when emotions shift very fast. They help reduce irritability and impulsive reactions. Basically, they help moods feel less extreme.
Antipsychotics
Antipsychotic medication is usually given only when symptoms are more serious. This can include severe anxiety, aggression, or confusing thoughts. Not everyone needs this, but it can help in some cases.
So overall, medication is more like support. It helps manage symptoms, while therapy does the deeper work over time.
Supportive Approaches
Supportive approaches really help people with personality disorders in their day-to-day lives. It’s not the main treatment, but it makes therapy and medicines work better. Helps with coping, feeling steady, and just getting through this.
Group Therapy
It’s a place to talk with others, practise how to communicate, and figure out better ways to deal with people.
Peer Support
Talking to people who’ve been through similar things can make you feel less alone. Also helps you feel like you’re not the only one struggling.
Crisis Management
Having a plan for when emotions hit hard is super important. Helps stay safe and not get completely overwhelmed.
Lifestyle Changes
Things like sleeping okay, exercising, chilling out, and cutting down on alcohol or drugs can really help with moods and emotions.
When you put therapy, medication, and supportive stuff together, people can actually start feeling better. It takes time, sometimes a lot, but steady support helps build better habits and makes life a bit more balanced.
Conclusion
Personality disorders can significantly influence how a person thinks, feels, and interacts with others, but understanding them helps reduce stigma and encourages early support. Recognising the symptoms, causes, and treatment options allows individuals and families to approach these conditions with more clarity and compassion.
Personality disorders can make life hard for a long time, but people can get better. With the right diagnosis, therapy, and support, a lot of individuals figure out healthier ways to handle emotions, deal with relationships, and manage everyday stuff. If more people understand these disorders and respond with kindness instead of judgment, it makes it easier for someone to ask for help and actually work toward feeling better.

FAQs
What are personality disorders?
Personality disorders are patterns in the way someone thinks, feels, and behaves that stick around for a long time. They can make everyday life harder to manage. These patterns often affect how someone sees themselves, how they connect with others, and how they control their emotions. People might react more strongly than they want, have trouble talking to others, or feel like no one really understands them. Usually, these behaviours start early in life and just keep showing up over time.
What causes personality disorders?
Personality disorders don’t happen because of one thing. It’s usually a mix of your genes, your childhood, and stuff that happened growing up. Trauma, a chaotic family, neglect, or losing someone important can make it harder to handle feelings. Brain differences or just the way someone naturally is can also play a role. Most of the time, it’s all these things together over the years that shape how someone thinks, feels, and acts.
Can personality disorders be cured?
There’s no quick fix or complete cure. But things can get better. Therapy helps, learning ways to cope helps, and having people around who support you really helps too. Many people figure out how to handle their feelings, deal with others better, and have a more stable life. It takes time, and it’s not always easy, but it is possible if you stick with it.
How are personality disorders treated?
Treatment usually focuses on therapy. It helps people understand their emotions and find better ways to handle them. There are different types, like CBT, DBT, MBT, schema therapy, and psychodynamic therapy, each of which offers tools for coping with challenges. Medicine can be added too, mainly for symptoms like anxiety, depression, or mood swings. Supportive approaches, like group therapy or small lifestyle changes, also help a lot.
Are personality disorders treatable without medication?
Yes, many people manage personality disorders successfully through therapy alone. Psychotherapy is the main treatment because it teaches long-term emotional and behavioural skills. Medication is only used when symptoms like depression, anxiety, or impulsivity need extra support. Some individuals may never need medication at all. What matters most is finding the treatment approach that works best for each person.
Can someone with a personality disorder live a normal life?
Yes, a lot of people can. Life can still be meaningful and stable. Therapy helps, and learning ways to cope makes things easier. Having friends or family who support you matters a lot, too. It takes time, and it’s not always smooth, but it can happen. Many people start to understand themselves better and build habits that actually work for them.







